Single Cell Immune Profiling and the Hunt for Unconventional Immune Cells
Single cell immune profiling reveals previously uncharacterized cytotoxic immune cells in studies of successful aging and neurodegenerative disease.
Scientists face the challenge of locating and defining the diverse immune cells that continuously patrol the human body. These immune cells are dynamic: they can travel to different parts of the body via the bloodstream and lymphatic vessels, and react to the environments they encounter, driving inflammation or differentiating to take on new roles. Established tools to study the immune system have paved a way into this complexity. For example, cytometry offers the powerful ability to determine cell-surface marker expression and group cells, while immunohistochemistry contributes a spatial dimension to marker expression. However, to truly define the phenotype and function of immune cells within a biological system or disease state, there is a need to gather deep insights into the immune repertoire and comparative gene expression at single cell resolution. Here, we highlight a few research stories where these methods were combined to discover some unconventional immune cells and how they operate in aging and disease.
Supercentenarians Have Higher Numbers of Cytotoxic CD4 T Cells
Is this the secret to long life? Kosuke Hashimoto and colleagues from the Riken Center for Integrative Medical Sciences, and the Centre for Supercentenarian Medical Research in Japan, sought to understand the quality and activity of the immune system in individuals who have reached the amazing age of 110 years. They noted that the aging process typically entails a gradual decline in immune functions and the onset of lethal diseases, like cancer or stroke. However, supercentenarians seem to have evaded this decline, suggesting their immune systems remain active.
Researchers used single cell RNA-sequencing (scRNA-seq) to profile blood samples from 7 supercentenarians and 5 younger controls, identifying 10 clusters that represent the major cell types of PBMCs. Comparing supercentenarians and controls, they observed two populations of T cells that were imbalanced: one population was diminished in supercentenarians while the other was expanded. Further analysis of the gene expression data in these two cell groups using Seurat revealed that the first group expressed genes associated with naïve and central memory T cells, while the second, expanded group expressed multiple genes encoding cytotoxic effector molecules. This evidence suggested that cytotoxic T cells were significantly expanded in supercentenarians, reaching 80% of T cells in some subjects.
Unexpectedly, however, these were not all CD8+ T cells. Gene expression data suggested a significant subset were actually CD4+ cytotoxic T lymphocytes (CTLs). The researchers constructed single cell trajectories using the Monocle 2 (version 2.4.0) R package to understand how these CD4+ T cells could arise in the context of differentiation. This analysis showed that CD4 CTLs arose in later pseudotime, and were accompanied by a gradual increase of expression of GZMA, GZMB, and PRF1, which encode cytotoxic molecules. They then performed single cell T cell receptor (TCR) repertoire analysis, and noted that the cell state transition of these CD4 CTLs could be explained by clonal expansion after stimulation from an antigen, possibly through repeated viral exposure. Though the potential role of CD4 CTLs in tumor immunity and immunosurveillance remains undefined, these findings point to unique and unconventional adaptations that may allow successful aging in supercentenarians (1).
Brains Affected by Neurodegeneration Show Proinflammatory CD8 T Cells in the CSF
This may be the first time that clonally expanded CD8+ T cells have ever been observed in the ventricular pathways of the brain. In an effort to shed light on the role of the adaptive immune system in driving the neuroinflammatory symptoms of Alzheimer’s disease (AD) and other neurodegenerative diseases, David Gate and colleagues from Stanford University studied blood samples from affected patients. Using mass cytometry, they identified an expanded population of CD3+ CD8+ CD27− T effector memory CD45RA+ (TEMRA) cells, which were shown to have potent effector functions, including the ability to secrete proinflammatory cytokines. Analysis by scRNA-seq showed that these CD8+ TEMRA cells had increased TCR and cytokine signaling, suggesting they experienced greater antigenic stimulation in patients with AD compared to controls.
These intriguing qualities led the team of researchers to explore the spatial localization of TEMRA cells in the post-mortem brains of patients with AD. Using immunohistochemistry, they mapped the expression of genes that would indicate CD8+ T cells and amyloid beta plaques, and detected distinct colocalization, as well as CD3+ CD8+ T cells in the leptomeninges—that is, the inner two meninges, thin stretches of membrane that protect the brain and spinal cord, through which flows cerebrospinal fluid (CSF).
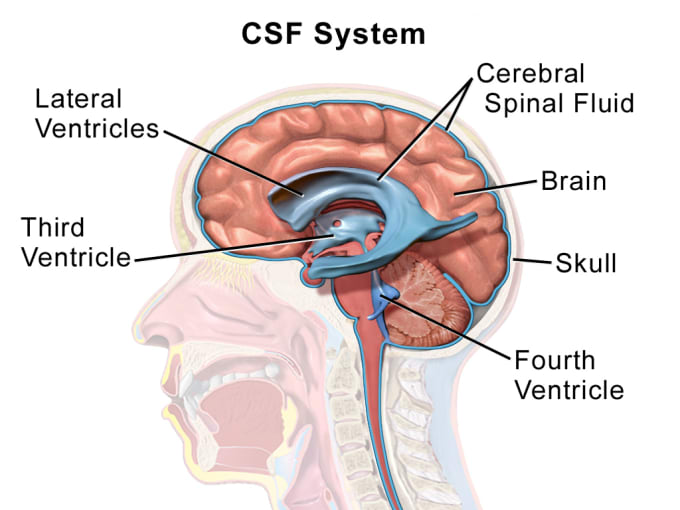
This finding led them to question if these T cells also patrol the CSF. Further testing of the CSF in a new cohort of healthy elderly controls and AD patients revealed that the CD8+ T cell repertoire of CSF from elderly individuals was composed almost exclusively of T effector memory (TEM) cells, including about 20% TEMRA cells; and notably, one AD patient had a massively expanded CD8+ CD45RA+ CD27− TEMRA clone.
To further characterize the clonal repertoire of T cells found in the CSF collected from elderly cohort subjects, researchers performed single cell TCR-sequencing. They observed numerous highly expanded CD8+ clones—meaning more than five T cells with the same TCRαβ sequence—in patients with AD. They noted that 49.13% of these clones were CD8+ TEMRA cells. Subsequent differential gene expression analysis showed that CD8+ TEMRA clones had increased expression of cytotoxic effector genes and proinflammatory cytokines associated with AD; and MHC genes, including beta-2-microglobulin (B2M), a known pro-ageing factor that impairs cognition.Together, this rich data points to a proinflammatory, cytotoxic function of clonal CD8+ TEMRA cells in the CSF of patients with AD (2).
Other researchers have been studying T cell infiltration in the aging mammalian brain using single cell RNA-sequencing. Read this publication from Nature to find out more about the unconventional immune cells this team of researchers discovered (3).
These unconventional immune cells and the process that led to their discovery demonstrate the importance of asking questions in response to unusual biological circumstances and conducting subsequent exploratory research. With the combined power of established immunological methods and single cell immune profiling, it is increasingly possible to define the complex immune cells that perform critical roles in the story of health and disease—and to leave no stone unturned in the search for more unconventional cells.
Learn more about single cell immune profiling →
Explore cutting-edge science conducted with 10x Genomics technology in our publications database →
- K. Hashimoto et al., Single-cell transcriptomics reveals expansion of cytotoxic CD4 T cells in supercentenarians. PNAS. 48, 24242–24251. (2019).
- D. Gate et al., Clonally expanded CD8 T cells patrol the cerebrospinal fluid in Alzheimer's disease. Nature. 577, 7790. (2020).
- B. Dulken et al., Single-cell analysis reveals T cell infiltration in old neurogenic niches. Nature. 571, 7764. (2019).
